Sexhormones For Research
Abstract
Sex hormone is a steroid hormone secreted by the human body, through many physiological functions to regulate human life activities. At present, sex hormones, and sex hormone regulators have been widely used in the market, and with more patent medicine possibilities, the expansion of the treatment field is still under research. The development of sex hormone-related products is still in the stage of rapid development, our company provides a large number of related high-quality products for scientific research, for the sex hormone-related field of medical research and development workers to provide a solid material foundation.
What is Sexhormones?
Sex-hormone (lipids in nature) is a hormone synthesized from the gonads, placenta, adrenal reticular zone, and other tissues of animals, which is responsible for promoting the maturation of sexual organs, the development of secondary sexual characteristics, and the maintenance of sexual function. The ovaries of female animals mainly secrete two kinds of sex hormones – estrogen and progesterone, while the testis of male animals mainly secretes androgen, which is mainly testosterone.
Kinds of Sexhormones
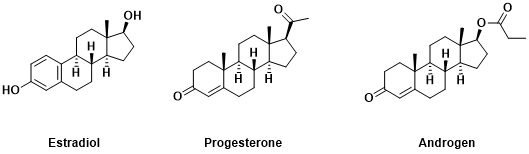
Figure 1 Structures of Sexhormones
Oestrogen
Oestrogen (also known as Estradiol) has the strongest activity among estrogenic steroid hormones, which are mainly synthesized in the granulosa cells of ovarian follicles, and estrone and estriol are their metabolites[1]. The 2-hydroxyl and 4-hydroxyl derivatives of estradiol also have important physiological significance. Since the discovery of the non-steroidal structure and estradiol-like compounds – ethyl phenol (trans-4, 4 ‘-2 hydroxy-α, β-diethyl) in 1938, more than thousands of analogs have been synthesized. Recently, tri-styrene derivatives have been developed. Some of these compounds can be used as estrogen substitutes or anti-estrogens. These compounds have a spatial configuration similar to estradiol and are easy to synthesize. In addition to certain clinical application values, they can also provide clues for the study of the principle of estrogen action[2]. However, its metabolism is different from that of steroid compounds, and its overall effect is complex, so it should be used with caution.
The synthesis of estradiol varies periodically, and its effective concentration is extremely low, with only micrograms/ml in the blood of humans and commonly used experimental animals such as rats and dogs. The target tissues of estrogen are the uterus, fallopian tube, vagina, and pituitary gland. The main function of estrogen is to maintain and regulate the function of accessory sex organs. In the early years, the changes of the accessory sexual organs of the ovariectomized animals were observed, and compared with the animals supplemented with exogenous estradiol, it was found that under the influence of estrogen, the activity of the fallopian tube and uterus increased, the atrophied uterus recovered, and the glands, stroma, and muscle parts were hyperplasia, uterine fluid increased, vaginal epidermal cell hyperplasia, and surface layer keratosis[3]. It has been found that not only classical target tissues have estrogen receptor proteins, but also many important central or peripheral organs such as the thalamus, pineal gland, adrenal gland, thymus, pancreas, liver, kidney, etc., have different amounts of receptor or binding protein molecules. Exogenous estrogen can cause changes in systemic metabolism. Large doses of estradiol can promote protein anabolism, reduce the use of carbohydrates, cause hyperlipidemia, and high cholesterol in birds, and therefore have an effect on fat metabolism. In addition, estradiol in tissues also has a certain effect on the retention of water and salt molecules and the maintenance of calcium balance. Estrogen also plays an important role in the sexual differentiation of the central nervous system. As its 2-hydroxyl or 4-hydroxyl derivatives belong to catechols, they can compete with catecholamine and other neuromodulators for enzyme systems, thus restricting and regulating each other and forming a bridge between the nervous system and the endocrine system. Further research in this regard may help to elucidate the neuroendocrine regulation mechanism of sexual differentiation, sexual maturation, sexual behavior, and reproductive function[4]. Various forms of estrogen derivatives have been widely used in contraception, treatment of menopausal syndrome in women, men’s prostatic hypertrophy, and other endocrine disorders.
Progestational Hormone
Progesterone is the most powerful progesterone and is the precursor substance of many steroid hormones, which is formed by the luteum after ovulation of the follicle of the mammal ovary and the hormone secreted by the placenta. Its main function is to make the accessory sex organs of mammals for pregnancy preparation, embryo implantation in the uterus, and maintaining pregnancy essential hormones[5]. Progesterone is widely distributed and is synthesized in the ovaries of non-mammals such as birds, sharks, lungfish, starfish, and cuttlefish. Such as bird oviduct egg albumin production that fertility ketone activation.
The combined action of progesterone and estrogen in the body ensures the normal process of menstruation and pregnancy. Estrogen promotes endometrial thickening and endometrial vascular hyperplasia. After ovulation, progesterone secreted by the corpus luteum acts on the uterus and mammary gland initially activated by estradiol, weakening the contraction of the myometrium, hyperplasia of the glands, blood vessels, and epithelial tissues of the endometrium, and showing secretory changes. Progesterone causes hyperplasia of breast acinus with well-developed ducts. These effects also depend on progesterone receptors in the cytoplasm, whose synthesis is induced by estradiol[6]. Progesterone has few other functions in higher animals. It is known that large doses of progesterone can cause a male reaction, and pharmacological doses of progesterone can also inhibit the secretion of the pituitary sex hormone. The ovulation inhibition effect of progesterone contained in contraceptives is the result of inhibiting the gonadotropin.
Androgen
Androgens are secreted by the testis, ovaries, and adrenal glands. Testosterone is the most important androgen produced by the testicles. Androgen acts on male accessory sexual organs, such as the prostate and seminal vesicle, to promote their growth and maintain their functions[7]. It is also an indispensable hormone for maintaining male accessory sexual characteristics, such as the crown of poultry, feathers of birds, horns of ruminants, hair, and the Adam’s apple of human beings. Androgens also promote systemic anabolic metabolism and enhance nitrogen retention, especially in the liver and kidneys[8].
Androgens are widely distributed in the animal kingdom and are 19-carbolic compounds. There are a large number of synthetic androgens, including esterification, methoxylation, or fluorinated derivatives, which are easy to take orally or have a strong anabolic function and can be applied in clinical practice.
Unlike estrogen, androgen secretion has no obvious periodicity, but it also forms a feedback relationship with pituitary gonadotropin. Testosterone is a form that runs in the blood and is responsible for the feedback effect, but when it works at the cellular level, testosterone often needs to be converted into dihydrotestosterone, which has a higher affinity for binding to receptor proteins than testosterone[9]. Another way androgens are transformed at the cellular level in tissues such as the hypothalamus is through the aromatization of the A-ring to form estrogen, resulting in very high levels of estrogen in the testes of some animals. This transformation in the central nervous system is important in the sexual differentiation of the brain.
Functions of Sexhormones
Although the physiological effects of hormones are very complex, they can be summarized into five aspects:
First, it provides energy for life activities and maintains the dynamic balance of metabolism by regulating the metabolism of protein, sugar, and fat as well as water and salt.
Second, promote cell proliferation and differentiation, affect cell senescence, and ensure the normal growth and development of tissues and organs, as well as cell renewal and senescence. For example, growth hormone, thyroid hormone, sex hormone, and so on are hormones that promote growth and development.
Third, to promote the development and maturity of reproductive organs, reproductive function, as well as the secretion and regulation of sex hormones, including a series of reproductive processes such as ovulation, ovulation, spermatogenesis, fertilization, implantation, pregnancy, and lactation.
Fourthly, it affects the development and activity of the central nervous system and vegetative nervous system, and the relationship with learning, memory, and behavior[10].
Fifth, closely cooperate with the nervous system to adjust the body’s adaptation to the environment.
It is difficult to separate the roles of the above five aspects from each other, and regardless of the role, hormones only act as messengers, transmitting information about certain physiological processes, speeding them up or slowing them down, and cannot cause any new physiological activities.
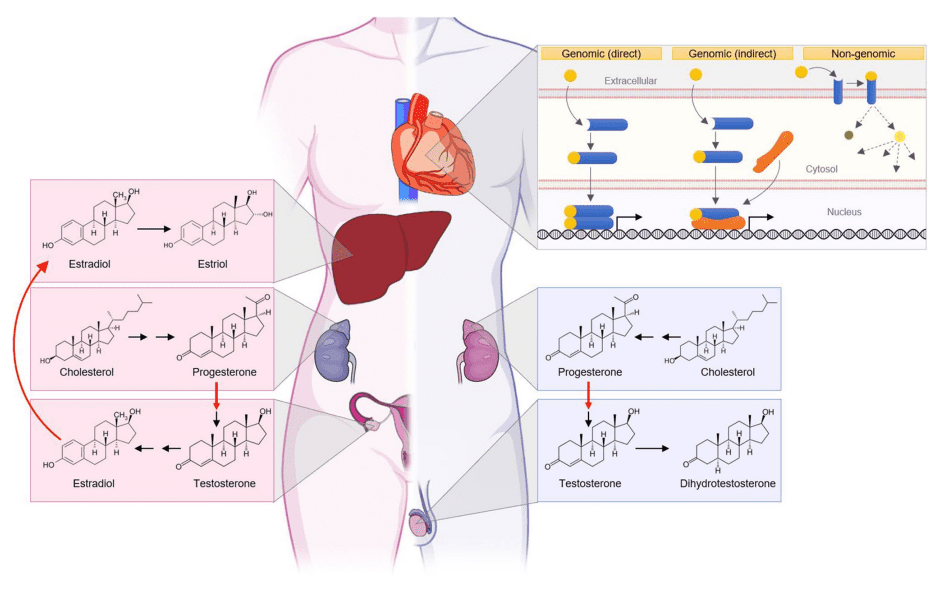
Figure 2 Sexhormones in human body
Sex hormones only have specific effects on certain tissues or cells (called target tissues or target cells). Every kind of tissue and cell in the human body can be the target of this or that hormone. For each kind of hormone, one or several tissues and cells can be selected as the target tissues or cells of this hormone. For example, growth hormones can play a unique role in bones, muscles, connective tissue, and internal organs, making the human body grow tall and strong. But muscles also act as targets for androgens and thyroxine[11,12].
Sex hormones act at the molecular level in the same way as other steroid hormones. They enter cells and bind to specific receptor proteins to form hormone-receptor complexes, which then bind to the nucleus and act on chromatin, affecting DNA transcription activities, leading to new or increased biosynthesis of existing proteins, and thus regulating cell metabolism, growth, or differentiation. Sex hormones are small molecules with lipid solubility. They enter cells mainly through free diffusion (passive transport), bind to cytoplasmic receptors, and form the hormone-cytoplasmic receptor complex. They acquire the ability to enter the nucleus through conformational change and heat shock protein dissociation and transfer from cytoplasm to the nucleus[13]. This triggers the process of DNA transcription, producing specific mRNA, which then enters the cytoplasm and is translated into proteins in the ribose body for biological effects.
Periodicity and stage of sex hormone secretion Due to the body’s periodic changes in the geophysical environment and long-term adaptation to the social living environment, hormone secretion produces an obvious time rhythm, hormone concentration in blood also presents a day, month, or year as the cycle of fluctuations. This cyclical fluctuation has nothing to do with fluctuations caused by other stimuli and may be controlled by the central nervous system’s “biological clock”.
The pattern and concentration of sex hormones in the blood After secreting hormones into the blood, part of the free form with the blood, the other part of the protein binding, is a reversible process. That is, free type + binding protein binding type, but only free type is biologically active. Different hormones bind to different proteins in different proportions. Conjugated hormones are metabolized and excreted by the kidneys longer than free ones, which prolongs the duration of hormone action. Thus, conjugated forms can be thought of as temporary deposits of hormones in the blood. Hormone concentration in the blood is also an indicator of the endocrine gland function activity state, it remains relatively stable. If the concentration of hormones in the blood is too high, it often means that the endocrine glands or tissues secreting this hormone are hyperactive; If it is too low, it indicates low or insufficient function.
Sexhormones drugs
Estrogen drugs
The natural estrogen drugs are Estradiol, Estrone, and Estriol and clinically common products can be taken orally or long-acting, such as Ethinylestradiol, Quinestrol, Estradiol valerate, Nierestrol, Diethylstilbestrol, Hexoestrolum, chlorotrianisene, etc.
- Inadequacy of female hormone secretion: ovarian hypoplasia or hypofunction.
- Menopausal syndrome: Appropriate supplement estrogen, can feedback inhibition and secretion, and reduce the symptoms.
- Contraception: large doses of estrogen can inhibit the secretion of FSH and achieve a contraceptive effect.
- Breast cancer: It is used for advanced breast cancer more than 5 years after menopause. It should not be used for patients within 5 years of menopause, otherwise, it will promote tumor growth.
- Other: Estrogen can increase bone calcium deposits, which can be combined with androgens to treat senile osteoporosis. Acne (acne) is often excessive androgen secretion of the sebaceous glands, causing blockage and secondary infection, so the use of estrogen antiandrogen treatment is. Estrogen also has the effect of elevating leukocytes, which can be used to treat leukopenia caused by radiation. It can enhance learning and memory in the elderly and delay the development of Alzheimer’s disease.
Pregnancy-hormone drugs
Natural progesterone for progesterone (progesterone), the body content is very little, and clinical use of its artificial products. There are mainly MedroxyProgesterone, Megestrol, Chlormadinone Acetate and hydroxyprogesterone caproate, Norethindrone, Evonorgestrel, NorethistereneAcetate, EtnynodiolDiacetate, etc[14].
It is mainly used for two purposes: contraception alone or in combination with estrogen (see Contraceptive section); Combined with estrogen for postmenopausal replacement therapy.
- Aura and habitual abortion: mainly using progesterone placenta effect, the effect of habitual abortion is not as good as aura abortion. Demethylated testosterone has an androgenic effect that masculinizes female fetuses.
- Functional uterine bleeding: The treatment of irregular exfoliation caused by insufficient progesterone, endometrial dysplasia, or continuous stimulation of estrogen endometrial hyperplasia caused by uterine bleeding.
- Diagnosis and treatment of amenorrhea. Progesterone is used to diagnose estrogen secretion and to understand the responsiveness of the endometrium to hormones. Withdrawal bleeding occurs if the endometrium reacts to endogenous estrogen 5 to 7 days after progesterone administration in amenorrhea. Estrogen and progesterone are also used in combination to diagnose and treat amenorrhea.
- Primary dysmenorrhea: Dysmenorrhea is caused by the synthesis of PGF2α in the endometrium by progesterone, which stimulates spastic contraction of the uterine muscle. 19- demethylated testosterone progesterone can inhibit luteal phase luteal secretion, thereby reducing dysmenorrhea.
- Endometriosis: Large doses can atrophy the endometrial glands to treat endometriosis and endometrial adenocarcinoma.
- Pictures of benign prostatic hypertrophy and prostate cancer: cancer feedback to inhibit adenohypophysis to secrete gonadotropin, reduce testosterone secretion, and treat prostatic hypertrophy and prostate cancer. As a palliative measure for metastatic endometrial carcinoma; Megestrol acetate is used as a second-line treatment for breast cancer.
Androgen Drugs
The natural androgen is testosterone. The clinical applications are synthetic testosterone and its derivatives, such as methyltestosterone[15], testosterone propionate, and testosterone phenylacetate.
- Inadequacy: testicular insufficiencies, such as no testis or similar testis.
- Functional uterine bleeding: mainly through the anti-estrogen effect, the uterine muscle fibers and blood vessels contract and endometrial atrophy and play a hemostatic role, especially suitable for menopause. Clinical use of tri hormone (a mixture of diethylstilbestrol, progesterone, and testosterone propionate) injection, generally can stop bleeding, but withdrawal bleeding can occur after withdrawal.
- Menopausal syndrome and uterine fibroids: use of its anti-estrogenic effect.
- Migratory breast and ovarian cancer can temporarily relieve symptoms, which may be related to its anti-estrogen effect. It may also reduce estrogen production by the ovary by feedback inhibiting the secretion of adenohypophysial gonadotropin.
- It is used for anemia, aplastic anemia, post-operative or various long-term wasting chronic diseases, and senile osteoporosis.
Sexhormones Regulator Drugs
A glycoprotein hormone that regulates gonad development in vertebrates and promotes the production and secretion of sex hormones. For example, luteinizing hormone (LH) and follicle-stimulating maturation hormone (FSH) secreted by the anterior pituitary gland work together to stimulate the development of germ cells in ovaries or testis and the production and secretion of sex hormones; Human placenta secretion of chorionic gonadotropin (HCG), can promote the secretion of progesterone luteum pregnancy. HCG appears in urine at the beginning of pregnancy and peaks in the second month of gestation. It is often used as a clinical indicator of pregnancy. Pituitary gonadotropin production and release are directly regulated by hypothalamic luteinizing hormone-releasing hormone (LH-RH)[16]. Sex hormones, the target gland product of LH and FSH, in turn, affect the secretory function of the pituitary or hypothalamus. Therefore, the secretion of LH-RH, LH, and FSH, as well as sex hormones, restricts each other and fluctuates rhythmically. LH is also known as interstitial cytotoxic hormone (ICSH) because it acts on the interstitial cells of the testes to stimulate the production and secretion of male hormones. The main effect of LH on the ovaries of female animals is to selectively induce the rapid growth of individual follicles before ovulation. When the secretion of LH reaches a climax, ovulation is triggered and the follicle wall after ovulation is transformed into the corpus luteum and the secretion of progesterone. The important role of FSH is to promote the growth and development of follicles in the ovary and, in males, to promote the production of sperm in the curved spermatogonium of the testis. Gonadotropin produced from the pituitary gland of animals has been widely used in animal husbandry and aquaculture, but it is ineffective for human beings. HCG can be prepared from the urine of pregnant women, or LH and FSH from the urine of menopausal women mixed preparation, referred to as human menopausal gonadotropin (HMG), can be used in the clinical treatment of hypersexual dysfunction.
Reference:
[1] Harborne, J. B., & Williams, C. A. (2000). Advances in flavonoid research since 1992. Phytochemistry, 55(6), 481-504.
[2] Vasudevan, N., & Pfaff, D. W. (2007). Membrane-initiated actions of estrogens in neuroendocrinology: emerging principles. Endocrine reviews, 28(1), 1-19.
[3] Revankar, C. M., Cimino, D. F., Sklar, L. A., Arterburn, J. B., & Prossnitz, E. R. (2005). A transmembrane intracellular estrogen receptor mediates rapid cell signaling. Science, 307(5715), 1625-1630.
[4] Rochester, J. R. (2013). Bisphenol A and human health: a review of the literature. Reproductive toxicology, 42, 132-155.
[5] Drummond, A. E. (2006). The role of steroids in follicular growth. Reproductive biology and endocrinology, 4, 1-11.
[6] Romero, R., Dey, S. K., & Fisher, S. J. (2014). Preterm labor: one syndrome, many causes. Science, 345(6198), 760-765.
[7] Burger, H. G. (2002). Androgen production in women. Fertility and sterility, 77, 3-5.
[8] Roy, A. K., Lavrovsky, Y., Song, C. S., Chen, S., Jung, M. H., Velu, N. K., … & Chatterjee, B. (1998). Regulation of androgen action. Vitamins & Hormones, 55, 309-352.
[9] Gelmann, E. P. (2002). Molecular biology of the androgen receptor. Journal of clinical oncology, 20(13), 3001-3015.
[10] Cooke, I. M., & Sullivan, R. E. (1982). Hormones and neurosecretion. The biology of Crustacea, 3, 205-290.
[11] Neave, N. (2007). Hormones and behaviour: a psychological approach. Cambridge University Press.
[12] Bouman, A., Heineman, M. J., & Faas, M. M. (2005). Sex hormones and the immune response in humans. Human reproduction update, 11(4), 411-423.
[13] Burrows, H. (2013). Biological actions of sex hormones. Cambridge University Press.
[14] Schiff, I., Tulchinsky, D., Cramer, D., & Ryan, K. J. (1980). Oral medroxyprogesterone in the treatment of postmenopausal symptoms. Jama, 244(13), 1443-1445.
[15] Bouchard, P. (2005). Chlormadinone acetate (CMA) in oral contraception–a new opportunity. The European Journal of Contraception & Reproductive Health Care, 10(sup1), 7-11.
[16] Burgus, R., Butcher, M., Amoss, M., Ling, N., Monahan, M., Rivier, J., … & Guillemin, R. (1972). Primary structure of the ovine hypothalamic luteinizing hormone-releasing factor (LRF). Proceedings of the National Academy of Sciences, 69(1), 278-282.